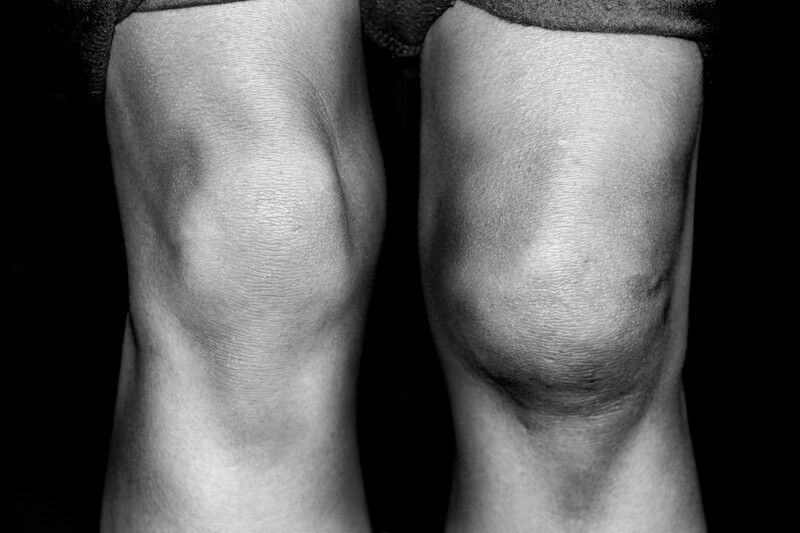
When a patient visits our practice with chronic joint pain, they will usually display a joint that is swollen, puffy, and painful. The fluid retention, especially in the knees will make walking, getting in and out of a chair or car, and daily living at best uncomfortable and, at worse, very painful. Managing inflammation can be a tricky thing. When we began offering non-surgical, non-medication, regenerative medicine therapies many years ago, we understood that inflammation was the body’s way to repair damaged tissue. Swelling in a joint not only signaled that the immune response was healing the damage, but the swelling in the joint itself acted as a brace or protective mechanism to hold the joint in place while it healed.
To the body’s thinking, swelling and inflammation must continue until the injury is healed. Of course in a patient with degenerative joint disease, the wear and tear stress on the joint is greater than the body’s ability to heal it. Chronic inflammation occurs as the immune system fights to heal damage that is beyond its ability to heal. The end result? A joint that is swollen, puffy, and painful. What to do with this inflamed joint is a matter a great debate in the medical community.
Conservative care of joint inflammation
Many patients that come into our office looking for joint pain relief and the ultimate avoidance of a joint replacement surgery, have already seen many doctors including orthopedists for a surgical consult. In many cases, a surgical recommendation will only be given following a robust and extensive pain management program to include the use of anti-inflammatories. Anti-inflammatory medication is seen as a way to shut off the chronic joint swelling and prevent further damage to the joint caused by chronic inflammation’s corrosive nature. Part of what inflammation does is to create a toxic wash that breaks down damaged tissue to make way for new tissue. When this toxic joint bath does not shut down, the joint remains awash in corrosive elements. This is why doctor’s express the greatest of urgency to get this inflammation to stop.
“Existing guidelines for pain management provide recommendations that do not satisfactorily address the complex nature of pain.”
Treating inflammation is a tricky thing. It is suggested that traditional medicine’s lack of a good way to treat inflammation leads to an “epidemic” of joint replacements. In October 2019, a paper (1) co-authored by researchers from the United States, Italy, France, Spain, and Germany offered these observation of the treatment of pain from inflammation.
“Existing guidelines for pain management provide recommendations that do not satisfactorily address the complex nature of pain. To achieve optimal outcomes, drug choices should be individualized to guarantee the best match between the characteristics of the patient and the properties of the medication. NSAIDs represent an important prescribing choice in the management of inflammatory pain, and the recent results on paracetamol (Tylenol) question its appropriate use in clinical practice, raising the need for re-evaluation of the recommendations in the clinical practice guidelines.
Increasing clinicians’ knowledge of the available pharmacologic options to treat different pain mechanisms offers the potential for safe, individualized treatment decisions. We hope that it will help implement the needed changes in the management of inflammatory pain by providing the best strategies and new insights to achieve the ultimate goal of managing the disease and obtaining optimal benefits for patients.”
So here in October 2019, researchers are saying there is a lot of problems with the way doctors are prescribing, using, and recommending anti-inflammatories for pain from inflammation.
Side note: Recently researchers have questioned the safety of Tylenol for treating pain related to chronic inflammation, especially in patients over 65. A study from April 2019 (2) offered this research conclusion: “Given that the analgesic benefit of paracetamol (Tylenol) in osteoarthritis joint pain is uncertain and potential safety issues have been raised, more careful consideration of its use is required.”
The controversy surrounding NSAIDs in people over 75
As pointed out NSAIDs have many side-effects. There is no controversy surrounding that. What is the controversy in older patients is just how bad these side effects may or may not be.
A June 2021 study (3) wrote:
“practitioners involved in the management of osteoarthritis often have to manage very old patients, aged 75-80 years and above . . .Treatment options are limited. In addition to education and physical treatments, which are at the forefront of all treatment recommendations but require a low level of symptoms to be implemented, many pharmacological options are proposed.
Nonsteroidal anti-inflammatory drugs (NSAIDs) can be used as a second-line treatment but with great caution. However, the precise incidence of cardiovascular, renal, and gastrointestinal adverse events in very elderly patients is unclear. All of these risks are increased in the elderly.
The researchers then asked: What are the absolute risks in this age group? The write: “The answer to this question is important because NSAIDs should be used in very elderly patients with osteoarthritis only if full information has been provided (to the patient) and the decision to prescribe this treatment is shared between the patient and their doctor. This article calls for “practical options and warnings to allow for a responsible and limited use of NSAIDs in the very old.”
A lot of recommendations, many you have tried and many have not worked for you.
In February 2020, the American College of Rheumatology and the Arthritis Foundation, updated their 2012 American College of Rheumatology recommendations for the management of hand, hip, and knee Osteoarthritis. This now titled 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee (4) examined available evidence for the treatment of osteoarthritis.
Here strong recommendations were made for among other treatments topical nonsteroidal anti-inflammatory drugs (NSAIDs) for knee osteoarthritis, oral NSAIDs, and intraarticular glucocorticoid (cortisone) injections for knee osteoarthritis.
For some people, these are recommendations that they have tried and these treatments did not help them. So where do these people turn?
Alternatives to anti-inflammatory medications and cortisone injections
For more than 30 years, the Magaziner Center has been leading the way in cutting-edge, non-surgical, regenerative medicine. The Center has successfully performed regenerative procedures on people of all ages and activity levels. Our treatments have enabled professional athletes to play again, weekend warriors to avoid joint-replacement surgery and patients regain lost mobility after a failed operation, accident or injury.
The procedures in which we specialize include:
Prolotherapy: A widely recognized orthopedic procedure that reconstructs joints, ligaments and tendons that have been weakened by trauma or arthritis.
Platelet-Rich Plasma Therapy: A way to jump-start the body’s natural healing process by delivering a high concentration of platelets directly into an injured area.
Regenerative Therapies: We utilize a variety of innovative therapies, including peptides, to help repair damaged tissue and restore normal cellular function.
We have many articles on this website which present alternatives to anti-inflammatory medications. They are listed below.
If you would like to explore more options to the treatments you have been given that are not working for you, please contact our office so we can start a conversation with you.
Researchers Say Knee Osteoarthritis Patients Need Vitamin D
Treating Joint Inflammation. The Problem With NSAIDs.
Researchers Say Knee Osteoarthritis Patients Need Vitamin D
Researchers Say Knee Osteoarthritis Patients Need Vitamin D
References
1 Varrassi G, Alon E, Bagnasco M, Lanata L, Mayoral-Rojals V, Paladini A, Pergolizzi JV, Perrot S, Scarpignato C, Tölle T. Towards an Effective and Safe Treatment of Inflammatory Pain: A Delphi-Guided Expert Consensus. Advances in therapy. 2019 Aug 16:1-20.
2 Conaghan PG, Arden N, Avouac B, Migliore A, Rizzoli R. Safety of paracetamol in osteoarthritis: what does the literature say?. Drugs & aging. 2019 Apr 1;36(1):7-14.
3 Cadet C, Maheu E, French AGRHUM Group (Association Geriatric and RHeUMatology). Non-steroidal anti-inflammatory drugs in the pharmacological management of osteoarthritis in the very old: prescribe or proscribe?. Therapeutic Advances in Musculoskeletal Disease. 2021 Jun;13:1759720X211022149.
4 Kolasinski SL, Neogi T, Hochberg MC, Oatis C, Guyatt G, Block J, Callahan L, Copenhaver C, Dodge C, Felson D, Gellar K. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis & Rheumatology. 2020 Jan 6.
1038
1308




































Recent Comments