An April 2021 paper in the Rhode Island medical journal (1) summarizes the current concerns regarding persistent post-Lyme treatment symptoms.
10-20% of individuals diagnosed with Lyme disease develop chronic symptoms after antibiotic treatment.
Study participants had mild impairments in physical and social functioning, mild symptoms of depression, anxiety, and sleep disturbance, and moderate pain interference, and fatigue . Participants reported greater symptoms than some other clinical samples including those with cancer and chronic pain. Post-hoc analyses revealed that women reported higher levels of fatigue than men.
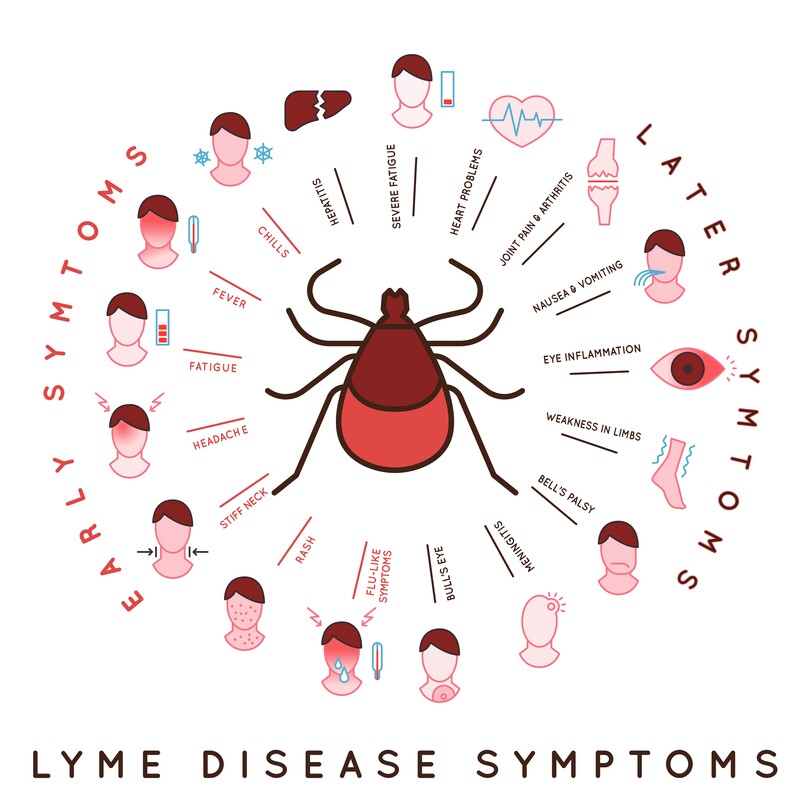
Research information like this is presented for doctors. It tells the doctors what they should look out for in people who have chronic complaint following Lyme Disease antibiotic treatment. Research like this is presented because chronic Lyme Disease symptoms can easily be overlooked or misdiagnosed. Acute exposure to Borrelia Borgdorferi, the spirochete that causes Lyme disease, may produce a “bullseye rash,” low grade fever, chills, fatigue, stiff neck, and muscle aches. However, chronic symptoms can include neurological complaints, bouts of arthritis, mild to severe fatigue, sleep disturbances, muscle aches, migratory joint pain or swelling, or difficulty concentrating, to name a few. Furthermore, testing is limited due to the “stealth” nature of the disease, and its ability to evade the human body’s natural immune system response. It is well known that traditional testing options have poor sensitivity and poor reliability.
March 2021: Lyme disease still controversial.
Above we just stated that chronic Lyme Disease symptoms can easily be overlooked or misdiagnosed. They can also be not that well understood. Let’s look at this study March 2021 (2) study to understand discussions doctors have among themselves when it comes to Lyme’s Disease.
“Persistent symptoms attributed to presumed tick-bite exposure constitute an unresolved medical controversy.”
In this study, doctors looked at 224 adults who met the criteria for post-treatment Lyme disease syndrome (symptoms persisted at least six months after treatment) and exhibited characteristics distinguishable from adults who did not, but who displayed similar symptoms and disease course after suspected previous tick-bite infection.
Each patient was examined by an infectious disease specialist and, besides a full medical history, underwent a panel of blood and cerebrospinal fluid laboratory tests including hematological, biochemical, microbiological and immunological analyses, and the RAND-36 scale to measure quality of life.
For analysis purposes, patients were divided into five subgroups, of which one group represented post-treatment Lyme disease syndrome
Conclusions: The post-treatment Lyme disease syndrome group did not differ exclusively in any respect from the other subgroups, which either lacked previously documented/reported evidence of borreliosis or even lacked detectable serological signs of exposure to Lyme disease. The results suggest that symptoms often categorized as Chronic-Lyme-Disease in the general debate, cannot be uniquely linked to Lyme disease. However, approximately 20% of the total group of patients showed signs of autoimmunity.
What does all this mean?
Conventional treatment options remain limited to antibiotics and are frequently prescribed for too short a course. Other inadequacies of traditional therapy include antibiotic-mediated disruption of gut flora, and the failure to address the various forms that the spirochete (a twisted bacteria) can morph into when it is under immune system attack. This ultimately allows the disease to further proliferate, despite completing course after course of antibiotic.
In order for Borrelia to survive, it requires collagen. To obtain this, it will activate the immune system’s cytokine response. This in turn, creates tissue inflammation, leading ultimately to a collagen rich environment that can promote the life cycle of the disease. This is why chronic Lyme disease symptoms are frequently associated with collagen rich regions of the body: joints, brain, muscles, eyes, and skin. Therefore, the goal of treatment is to calm down the body’s inflammatory response – that is to say, to calm down cytokine activity.
Through the traditional medical approach, a minimum of 3 weeks of antibiotic therapies are required to account for Borrelia’s lengthy life cycle. Extended antibiotic use, has been proven to be damaging to the gut microbiota, alternative therapies such as medicinal plants can be helpful to alleviate the body of Lyme, but are also safe for long term use, thus, sparing gut microbes, and may also help support the body’s immune system in the process. Several medicinal plants such as Andrographis, Resveratrol, and Chinese Skullcap, to name a few, have been researched to be antiviral, antibacterial, and antifungal. They can decrease the body’s inflammatory response, enhance natural killer cell function, and ultimately starve Borellia from its nutrient supply. Other therapies that we have found useful to stabilize symptoms of acute or chronic Lyme disease include hyperbaric oxygen, IV vitamin C, and activated oxygen therapy. Furthermore, addressing and supporting detoxification impairment, mitochondrial dysfunction, gut health, and neurological health are key to fully treating and alleviating symptoms of Lyme disease.
Is it ALS or Lyme Disease?
Below is a video of our patient Bob. Bob was diagnosed with Amyotrophic lateral sclerosis (ALS). As it turns out that was a misdiagnoses. The similarities and etiologies of Lyme Disease and ALS as well as other neurodegeneative disease is alluded to in a recent paper in the journal Current topics in medicinal chemistry. (3)
“Recent studies have shown that bacterial and viral infections are risk factors for various neurodegenerative diseases such as Amyotrophic lateral sclerosis, Multiple Sclerosis, Alzheimer’s disease, and Lyme disease. However, it is still controversial how the infections play a role in neurological diseases progression. Infections in central nervous system may lead multiple damages in infected and neighboring cells. The infection leads to the activation of inflammatory processes and host immune responses, which acts as defense mechanism and also causes damage to the host neuronal functions and viability. Several bacterial and viral pathogens have been reported for neurodegeneration, such as the production and deposit of misfolded protein aggregates, oxidative stress, deficient autophagic processes, synaptopathies and neuronal death.”
If you are experiencing symptoms that may be related to tick borne illness, contact the Magaziner Center for Wellness today and schedule an appointment.
1 Vargas SE, McCarthy M, Boudreau M, Canfield D, Reece R, Flanigan T. Characterizing the Symptoms of Patients with Persistent Post-Treatment Lyme Symptoms: A Survey of Patients at a Lyme Disease Clinic in Rhode Island. R I Med J (2013). 2021 Apr 1;104(3):53-57. PMID: 33789412.
2 Nilsson K, Skoog E, Jones V, Labbé Sandelin L, Björling C, Fridenström E, Edvinsson M, Mårtensson A, Olsen B. A comprehensive clinical and laboratory evaluation of 224 patients with persistent symptoms attributed to presumed tick-bite exposure. Plos one. 2021 Mar 18;16(3):e0247384.
3 Zubair Alam M, Alam Q, Amjad Kamal M, Ahmad Jiman-Fatani A, I Azhar E, Azhar Khan M, Haque A. Infectious agents and neurodegenerative diseases: exploring the links. Current topics in medicinal chemistry. 2017 May 1;17(12):1390-9.




































Recent Comments